 Osteoarthritis (OA) is one of the most common degenerative joint diseases worldwide, affecting approximately 27 million adults alone in the United States.1 Although not as disabling as rheumatoid arthritis, it is seven times more frequent in occurrence in the population. It is also one of the oldest recorded diseases in human history, showing up in the skeletons of Egyptian mummies and European descendants from centuries ago.
Osteoarthritis (OA) is one of the most common degenerative joint diseases worldwide, affecting approximately 27 million adults alone in the United States.1 Although not as disabling as rheumatoid arthritis, it is seven times more frequent in occurrence in the population. It is also one of the oldest recorded diseases in human history, showing up in the skeletons of Egyptian mummies and European descendants from centuries ago.
I will discuss the overview and treatment of OA in this article. A unique look at diet and lifestyle therapy, along with conventional medical therapy with drugs and surgery will be detailed here.
What is Osteoarthritis?
OA is a joint disorder that damages and destroys joints. The World Health Organization (WHO) estimates that 80% of people suffering from OA experience some form of limitation in movement, another 25% are unable to carry out important activities of daily life with this type of arthritis.
OA can occur in any joint in the body that allows free movement. It most commonly occurs in joints of the hip, knee, and spine, but also affects (to a lesser extent) joints of the shoulder, fingers, thumb, and large toe.
The severe pain and dysfunction resulting from OA is the result of a destructive inflammatory process that degrades the cartilage, bone, and tissues comprising the affected joint area.
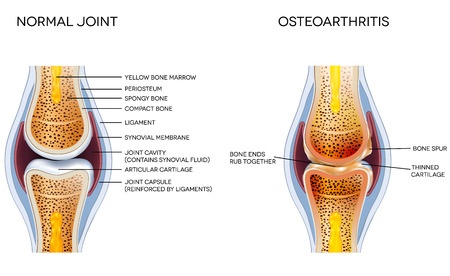 As you can see in the diagram, a normal, healthy joint is made of two or more bones joining together from opposite sides. The bones are separated by a fluid-filled space called the joint cavity. This cavity contains synovial fluid, which provides for the free-flowing movement of the joint. A thin layer of cartilage covers each end of the bone. Cartilage helps decrease friction upon movement and helps protect the bone by evenly distributing the forces exerted on it by load-bearing activity.
As you can see in the diagram, a normal, healthy joint is made of two or more bones joining together from opposite sides. The bones are separated by a fluid-filled space called the joint cavity. This cavity contains synovial fluid, which provides for the free-flowing movement of the joint. A thin layer of cartilage covers each end of the bone. Cartilage helps decrease friction upon movement and helps protect the bone by evenly distributing the forces exerted on it by load-bearing activity.
In OA, the cartilage becomes damaged and starts to erode, the underlying bone becomes damaged and starts to develop cysts, and fragments of cartilage are released into the synovial fluid causing inflammation.1 Eventually, the bone may become flattened, and the cartilage will become seriously degraded, if any is left at all. Bones will start to rub against one another and cause significant amounts of pain and suffering. This is what you may have heard others refer to as bone-on-bone pain.
OA may become so bad in some individuals that they have to undergo major joint replacement surgery (i.e. knee or hip replacement). This happens after the failure of medication therapy to effectively manage their symptoms when permanent joint damage has developed from their arthritis. After surgery, weeks to months of physical therapy follows. The average cost of surgery itself for knee and hip replacements is approximately $30,000 to $70,000 per surgery.2
What are the Risk Factors for Developing OA?
To date, no single cause has been identified as the determinant factor in causing OA. Instead numerous risk factors have been associated with the disease, many of which can be linked to diet and lifestyle habits. Known risk factors are listed below for OA:1
- Advanced age
- Female gender
- Obesity (BMI > 30)
- Cigarette smoking (men only)
- European descent (less common in Asians)
- Major trauma to joint
- Repetitive loading microtrauma to the joint
- Resective joint surgery
- Genetic factors (e.g. Heberden’s nodes in women, Ochronosis, Ehler-Danlos syndrome)
You can’t do anything to reduce risk factors such as aging, genetic predisposition, or accidental trauma to joints when trying to prevent OA. However, many of the above risk factors are influenced by diet and lifestyle, and you can do something about these.
Ethnicity might not even be a true risk factor, as it is noted in one review article that Asian individuals who adopt a Western diet (and the added weight that comes with it) increase their risk of OA, much like that of other Western cultures.1
The link between obesity and OA is well established.3 Being overweight or obese not only increases the frequency of OA in a population, but also influences the severity of the disease; obese individuals have significantly more joint degeneration in the knees than normal weight or underweight individuals. For every 5 kg of weight gain there is a 36% increase in risk of knee OA. Losing weight is key to reducing pain and severity of OA. This should be a primary goal of all patients with OA.
Treating OA With Medications
 After diagnosis is confirmed in OA, the typical approach with conventional medical treatments is listed below (in addition to physical therapy exercises for all patients).4,5
After diagnosis is confirmed in OA, the typical approach with conventional medical treatments is listed below (in addition to physical therapy exercises for all patients).4,5
*Note – each successive treatment is tried once the previous treatment fails.
- Tylenol
- Non-steroidal anti-inflammatory (NSAIDs – ibuprofen, napoxen, etc.)
- Corticosteroid injections and/or hyaluronic acid (gel-like) injections
- Opioids (hydrocodone, oxycodone, etc.) – may or may not be used in all patients
- Joint replacement surgery
Tylenol (Acetaminophen)
Success rate – In a 2006 Cochrane Review of five randomized controlled trials, a 5% improvement in baseline pain scores was achieved by acetaminophen use versus placebo.6 The numbers needed to treat (NNT) to improve pain for acetaminophen was between 4 and 16, meaning 4 to 16 patients needed to be treated with acetaminophen for one patient to experience the 5% improvement in pain relief.
Adverse effects – Acetaminophen is known to cause liver failure and/or liver damage at higher doses (> 4 g/day). There is also concern of kidney function impairment with higher doses of acetaminophen. Women with long-term use of acetaminophen exhibited mild loss of kidney function.1 Acetaminophen exhibits dose-related (> 3 g/day) gastrointestinal toxicities (risk of hospitalization from perforation, ulceration, or bleedings).1,7 Frequent (weekly or daily) use of acetaminophen has been linked to runny nose and asthma.
Non-Steroidal Anti-Inflammotory Drugs (NSAIDs – ibuprofen, naproxen, etc.)
Success rate – The NNT for ≥ 50% improvement in baseline pain scores for various NSAIDs (ibuprofen, naproxen, celecoxib) over a 4-week period is between 3.9 and 6.9.8 In other words, approximately 4 to 7 people have to be treated for 4 weeks for one person to experience ≥ 50% improvement in pain scores.
Adverse effects – NSAIDs are known to be more side-effect-prone than acetaminophen. Common adverse effects include gastrointestinal bleeding, worsening kidney function, and high blood pressure (numbers needed to harm [NNH]=12).4 The NNH means one person will experience one or more of these side effects for every 12 people treated with the drugs. Ibuprofen appears to be the safest of this group due to its shorter half-life, resulting in quicker removal from the body.9 Celecoxib (Celebrex) has less gastrointestinal side effects, but higher cardiovascular risk.4 Recently the FDA strengthened their warning that all NSAIDs increase the risk of strokes, heart attacks, and heart failure.10 The risk increases with higher doses and longer use.
Corticosteroid Injections
Success rate – Corticosteroid injections injected directly into the knee joint showed improvements in inflammation and pain with a NNT of 4.11 These improvements in symptoms were seen at the 1-3 week mark. Solid evidence for longer-term symptom improvement is lacking. Corticosteroid injections have not been shown to be as effective for shoulder or hand joints.4
Adverse effects – Corticosteroid injections into the joint cavity may produce pain at injection site, flare-up or worsening of arthritis (within 24 hours), skin pigment changes, loss of fatty tissue at injection site causing pitting, scarring, and bumps, or joint infection.12 A severe infection, known as a septic joint infection, has occurred following knee injection in 1 out of every 3,000-5,000 patients.
Hyaluronic Acid (gel-like) Injections
Success rate – Hyaluronic acid injections have been shown to be slightly better than or comparable to acetaminophen and NSAIDs in relieving symptoms in knee osteoarthritis.4,13 The injections start to take effect at 4 weeks, reach a peak effect at 8 weeks, and wear off at around 24 weeks.
Adverse effects – Acute local injection site reactions occur in 2-8% of patients.11
Opioids
Success rate – A 12% improvement in pain scores is experienced with the use of opioids versus placebo, with a NNT of 10.14 An 11% improvement in function is seen with the use of opioids versus placebo, with a NNT of 11.
Adverse effects – The improvements in symptoms with opioids comes with significantly more side effects than other medications used to treat OA. The number needed to harm is 5 for opioids.11 Adverse effects include a two-fold increased risk in delirium, 38% increased risk of bone fractures, 38% increase risk of pneumonia in elderly patients, increase in constipation, nausea, and dizziness in 20% of older patients, and increased risk of hospitalizations and mortality compared with NSAIDs.15
Joint Replacement Surgery
Success rate – Total joint replacement surgery is an option for those failing all other forms of therapy in severe OA. Functional improvement and pain relief is seen in 53%-90% of patients undergoing surgery.16 Much of the postoperative success will depend upon weeks to months of physical therapy and continued regular physical activity over the long term. Patients can expect their joint prostheses to function well for 15 to 20 years.4
Adverse effects – Joint replacement surgery is a major surgery requiring general anesthesia and hospital admission. Ninety-day postoperative complication rates for knee replacement surgery include: mortality (0.7%), hospital readmission (0.9%), pulmonary embolism [life-threatening blood clot in the lung] (0.8%), and wound infection (0.4%).11
Treating OA with Diet and Lifestyle

While many clinicians and patients are quick to resort to drugs and surgery when treating OA, there are effective non-medical treatment strategies to alleviate the pain and suffering too. These include the adoption of a whole foods, plant-based (WFPB) diet, weight loss, and regular exercise. While no treatment strategy has been known to reverse OA, these non-medical treatment options may provide some or all of the same benefits that medication therapy provides without any of the side effects.
Exercise
Success rate – Strength training programs designed specifically to increase muscular strength and joint stability have resulted in an 80% decrease in pain and significant improvement in range of motion.17 Physical therapy programs have shown to improve pain and function in 55%-58% of patients. Exercise also aids with weight loss too.
Adverse effects – None.
Weight Loss
Success rate – A weight reduction of 10% has been shown to improve function by 28% in OA patients.11 The Framingham study demonstrated that a 5.1 kg reduction in weight over a 10-year period decreased the likelihood of women developing symptoms of knee OA by 50%.3
Adverse effects – None.
Whole Foods, Plant-Based Diet
Many different dietary approaches have been taken to help alleviate pain and suffering in OA patients. Most diets focus solely on weight loss, without giving another thought to a person’s overall health. A WFPB diet not only helps individuals lose weight, but also improves their overall health by decreasing the risk of several chronic diseases (heart disease, type 2 diabetes, autoimmune diseases, cancer, etc.). This is why I encourage this approach over traditional dietary advice.
Success rate – A six-week, randomized, interventional study was undertaken comparing a WFPB diet versus a standard control diet (i.e. study participant’s normal diet) to reduce symptoms of OA.18 Patients were asked to rate their improvement in activity limitations, symptoms, emotions, and overall quality of life related to their OA throughout the study. A 50% increase in scores were seen in the WFPB group at week two. By week six, scores for the WFPB group had increased 100%, while the standard control group remained about the same.
Pain scores were also analyzed between groups on a visual pain scale of 0 = “no pain” to 10 = “worst imaginable pain.” Patients in the standard control group saw pain scores improve from 3.6 (week 1) to 2.4 (week 6). Patients in the WFPB group saw even better improvements in pain scores, despite starting out with more pain. The WFPB group pain scores improved from 5.1 (week 1) to 2.2 (week 6).
In addition, the WFPB dieters experienced improvements in weight, BMI, and blood pressure over the standard control diet group.
Adverse effects – None.
Summary and Final Thoughts
OA is a serious, debilitating disease. It can cause a great deal of pain and suffering for those affected by it. The debilitating effects can last for years, or even decades, in patients with OA. This is why it’s so important to be proactive in preventing OA by maintaining a healthy weight and staying physically active if possible.
If you do become diagnosed with OA, it’s still crucial to implement proper diet and lifestyle measures as soon as possible. Doing so will help preserve the remaining functioning of your affected joints. It will also help reduce pain and inflammation due to OA. Adopting a WFPB diet and a regular exercise program is key to accomplishing this.
When starting an exercise program specifically designed for OA, it’s important to reach out to a qualified medical professional (physical therapist, physician, etc.). You will get the proper exercises for your specific capabilities by doing so. After all, you wouldn’t want to further injure yourself by overdoing it or performing the wrong exercises based on what your joints can handle.
For those who need additional medical support for their OA, medications and surgery are available. Hopefully, by reading this article you are in a position to make a better-informed decision should you need to use these modalities.
With the right attitude and correct information, you can do a lot to stave off complications of OA. Your efforts will be worth it. I wish you all the best in your journey towards optimal health and a pain-free life!
Related articles:
Rheumatoid Arthritis – What Is It & How To Treat It
5 Exercises That Are Easy On Your Joints

If you like what you see here, then you’ll LOVE my daily Facebook and Twitter posts! Also, don’t forget to sign up for my Free Online Mailing List to get all the latest updates from the Plant-Based Pharmacist!
Check out my book, The Empty Medicine Cabinet, to start your journey towards better health. This step-by-step guide leads you through many of today’s common chronic diseases (heart disease, obesity, diabetes, cancer, and more), giving you the facts on food versus medication in treating these medical conditions. The book also contains an easy-to-follow guide on how to adopt a whole foods, plant-based diet as a part of an overall lifestyle change, producing the best possible health outcomes for you and your family. Hurry and get your copy today!
References:
1 Adatia A, Rainsford KD, Kean WF. Osteoarthritis of the knee and hip. Part I: aetiology and pathogenesis as a basis for pharmacotherapy. J Pharm Pharmacol. 2012 May;64(5):617-25.
2 BlueCross BlueShield. A study of Cost Variations for Knee and Hip Replacement Surgeries in the U.S. 2015 Jan 21. Available: http://www.bcbs.com/healthofamerica/bcbs_bhi_report-jan-_21_final.pdf. Accessed 2015 Aug 3.
3 Bliddal H, Leeds AR, Christensen R. Osteoarthritis, obesity and weight loss: evidence, hypotheses and horizons—a scoping review. Obes Rev. 2014 Jul;15:578-586.
4 Sinusas K. Osteoarthritis: Diagnosis and Treatment. Am Fam Physician. 2012 Jan 1;85(1):49-56.
5 Bruyere O, Cooper C, Pelletier JP, et al. An algorithm recommendation for the management of knee osteoarthritis in Europe and internationally: A report from a task force of the European Society for Clinical and Economic Aspects of Osteoporosis and Osteoarthritis (ESCEO). Seminars Arth and Rheu. 2014 Dec;44(3):253-263.
6 Towheed TE, Maxwell L, Judd MG, et al. Acetaminophen for osteoarthritis. Cochrane Database Syst Rev. 2006 Jan 25;(1):CD004257. Review.
7 Courtney P, Doherty M. Key questions concerning paracetamol and NSAIDs for osteoarthritis. Ann Rheum Dis. 2002;61:767–773.
8 Moore RA, Moore OA, Derry S, Peloso PM, Gammaitoni AR, Wang H. Responder analysis for pain relief and numbers needed to treat in a meta-analysis of etoricoxib osteoarthritis trials: bridging a gap between clinical trials and clinical practice. Annals of the Rheumatic Diseases. 2010;69(2):374-379.
9 Adatia A, Rainsford KD, Kean WF. Osteoarthritis of the knee and hip. Part II: therapy with ibuprofen and a review of clinical trials. J Pharm Pharmacol. 2012 May;64(5):626-36.
10 U.S. Food and Drug Administration. FDA Drug Safety Communication: FDA strengthens warning that non-aspirin nonsteroidal anti-inflammatory drugs (NSAIDs) can cause heart attacks or strokes. 2015 June 9; Available – http://www.fda.gov/Drugs/DrugSafety/ucm451800.htm. Accessed 2015 Aug 9.
11 Anandacoomarasamy A, March L. Current Evidence for Osteoarthritis Treatments. Therapeutic Advances in Musculoskeletal Disease. 2010;2(1):17-28.
12 Kruse DW. Intraarticular cortisone injection for osteoarthritis of the hip. Is it effective? Is it safe? Current Reviews in Musculoskeletal Medicine. 2008;1(3-4):227-233.
13 Bannuru RR, Natov NS, Dasi UR, et al. Therapeutic trajectory following intra-articular hyaluronic acid injection in knee osteoarthritis–meta-analysis. Osteoarthritis Cartilage. 2011 Jun;19(6):611-9.
14 da Costa BR, Nüesch E, Kasteler R, et al. Oral or transdermal opioids for osteoarthritis of the knee or hip. Cochrane Database Syst Rev. 2014 Sep 17;9:CD003115.
15 O’Neil CK, Hanlon JT, Marcum ZA. Adverse Effects of Analgesics Commonly Used by Older Adults with Osteoarthritis: Focus on Non-Opioid and Opioid Analgesics. The American journal of geriatric pharmacotherapy. 2012;10(6):331-342.
16 Losina E, Katz JN. Total joint replacement outcomes in patients with concomitant comorbidities: A glass half empty or half full? Arthritis and rheumatism. 2013;65(5):1157-1159.
17 Bhatia D, Bejarano T, Novo M. Current interventions in the management of knee osteoarthritis. Journal of Pharmacy & Bioallied Sciences. 2013;5(1):30-38.
18 Clinton CM, O’Brien S, Law J, et al. Whole-foods, plant-based diet alleviates the symptoms of osteoarthritis. Arthritis. 2015;2015:708152.


.jpg)
What if you are already on a plant-based diet and develop OA?
A plant-based diet does not reverse OA. It only helps reduce pain and suffering from it. If you are already plant-based then you may have to look into conventional or alternative therapies to treat OA.
What about the benefits of a plant-based diet for RA patients?